Overview
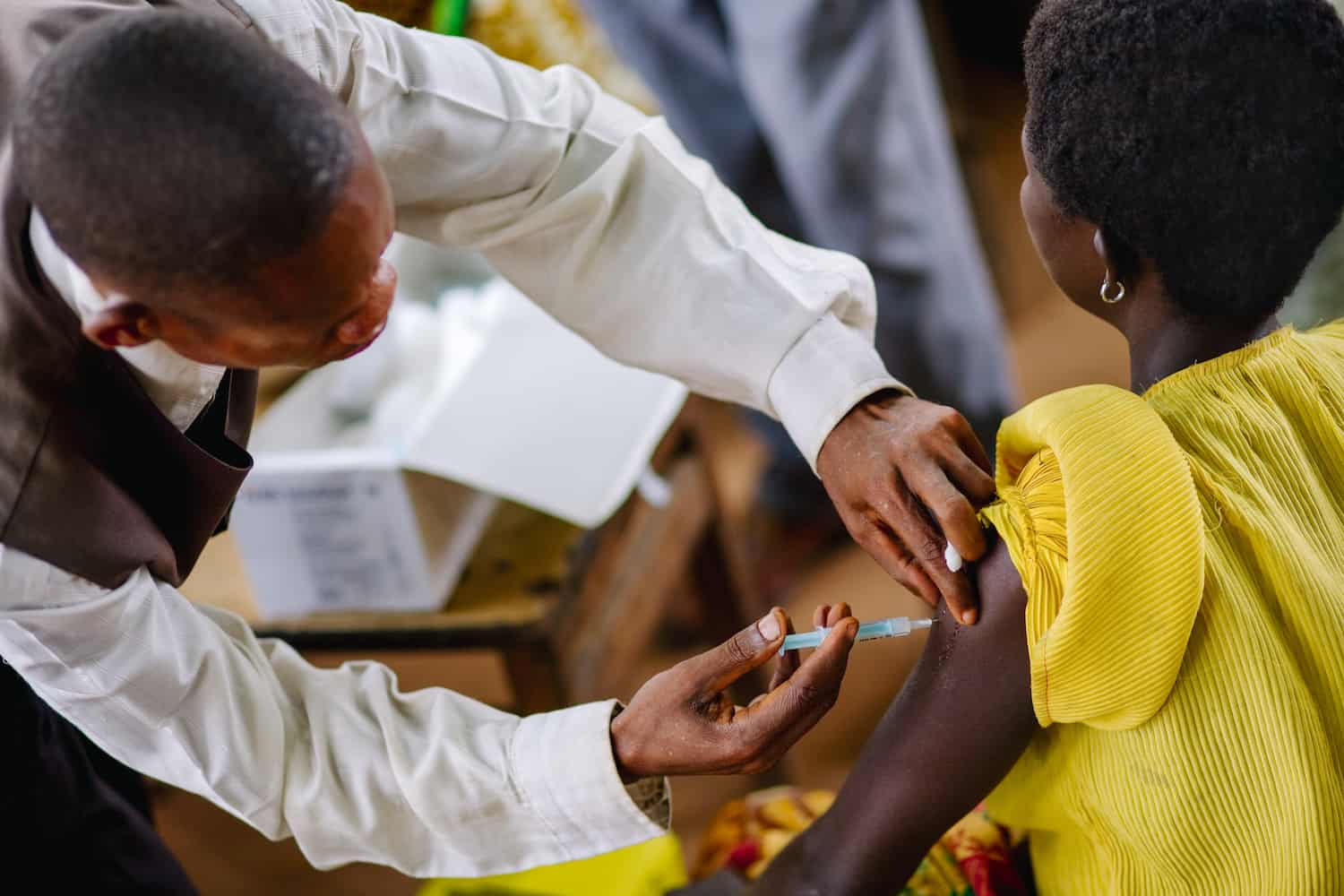
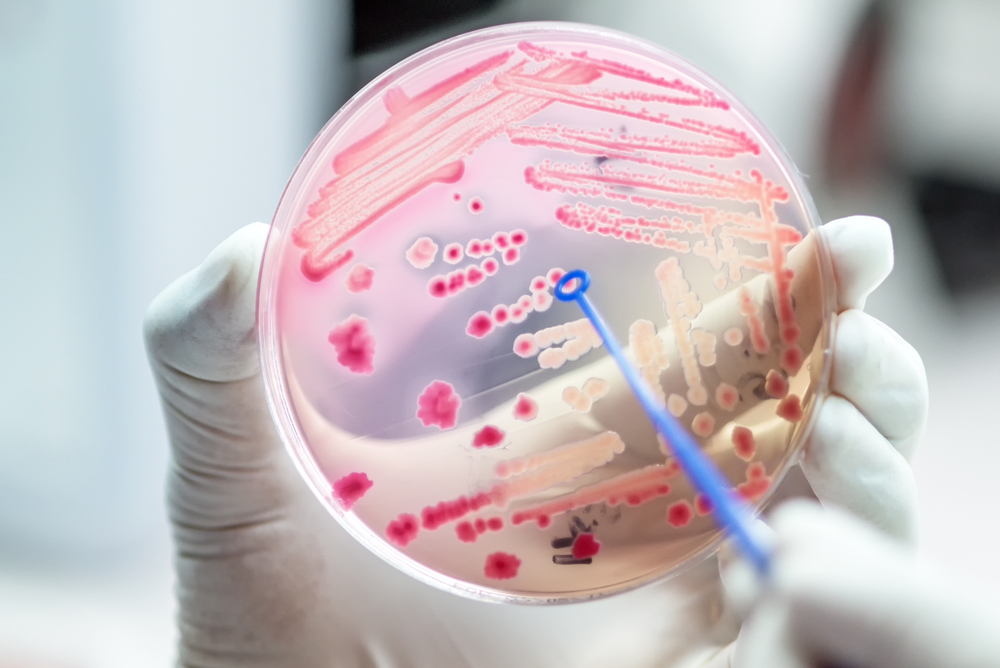
Antibiotic resistance disproportionately affects low- and middle-income countries with low levels of health care access, sanitation infrastructure, training for human and animal health care professionals, and public health education. In these countries, the Global Antibiotic Resistance Partnership (GARP) created a platform for developing actionable policy proposals on antibiotic resistance to address the disparities. GARP’s current focus lies in generating and communicating cross-disciplinary evidence describing the impact of vaccines on antimicrobial resistance (AMR) mitigation in country-specific contexts.
HISTORY
Since 2008, GARP has played a critical role in advancing country-led national strategies and policies to address AMR in 15 countries in Africa and Asia. The first stage of GARP included three phases of adding member countries into our network of partners to control the spread of drug resistance. Phase one of GARP, which ran between 2008 and 2011, included participants from India, Kenya, South Africa, and Vietnam. Between 2012 and 2015, Mozambique, Nepal, Tanzania, and Uganda joined the second phase. The third phase, which began in 2016, included the countries of Bangladesh, Laos, Namibia, Nigeria, Pakistan, Seychelles, and Zimbabwe.
In the first stage of GARP, we worked with member countries to contextualize AMR on national scales and provide policy recommendations to help meet World Health Organization goals for developing national action plans for AMR, and roadmaps for implementation. For stage two, we are currently working with member countries are working to highlight the role of vaccines in reducing the spread and emergence of AMR on local and regional levels.
GARP MODEL
At the heart of the GARP model is a technical working group of experts representing a range of disciplines in human, animal, and environmental health, ranging from academia and non-governmental organizations to faith-based organizations and the government. GARP country offices typically comprise of a chairperson, a co-chairperson, and a country coordinator, while in some countries, a principal investigator (PI) also joins the core team. Members of this core team, who are affiliated with prominent research institutions and universities in the member countries, facilitate regular interactions with technical working group members, and help organize webinars and in-person meetings on topics of relevance. The One Health Trust directly supports GARP activities in member countries both financially and logistically.
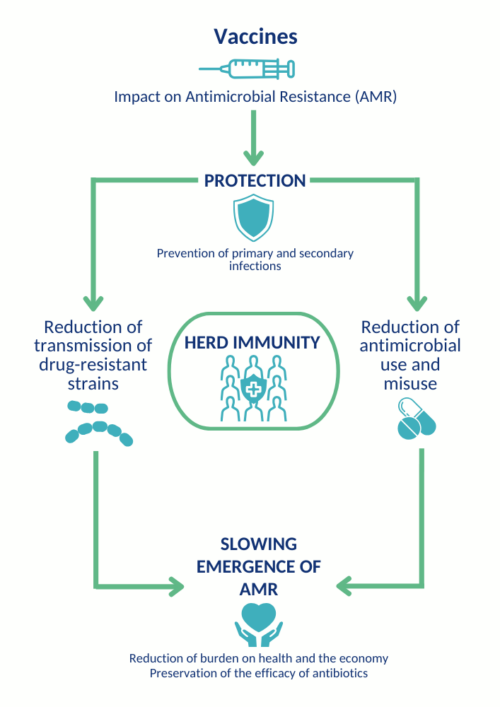
Vaccines and AMR
GARP’s current focus is generating and communicating cross-disciplinary evidence describing the impact of vaccines on AMR in country-specific contexts. Beyond infection prevention and reductions in mortality and morbidity, vaccines have the potential to mitigate AMR and limit its driving factors, which GARP wishes to highlight with the help of experts in its member countries. Countries currently part of this endeavour include Bangladesh, Kenya, Mozambique, Nepal, Pakistan, South Africa, Uganda, and Vietnam.

Outcomes
Since 2008, GARP member countries have produced several key deliverables which have been instrumental in informing national strategies to contain AMR. Some of the outcomes of GARP projects are described below.
SITUATION ANALYSIS
Since the network’s inception, GARP partners have developed situation analyses assessing human and animal antibiotic use and resistance, infectious disease burden, health indicators, pharmaceutical supply chains, and pertinent health regulations.
During the initial phases of GARP, such situation analyses were conducted in the countries of Bangladesh, India, Kenya, Mozambique, Nepal, Pakistan, South Africa, Tanzania, Uganda, and Vietnam. Links to these reports can be found below on the same page.
NATIONAL ACTION PLANS ON AMR
The situation analyses have informed the development of national action and implementation plans, produced in collaboration with and for the national governments.
AWARENESS AND EDUCATION
GARP working groups became focal points for many activities drawing attention to the AMR threat. Activities included antibiotic awareness weeks, research on appropriate antibiotic use and AMR surveillance, and the development of school curricula.
WEBINARS WITH KEY STAKEHOLDERS
In the current stage of GARP, technical working group members meet at regular intervals to discuss issues relevant to the subject of leveraging immunization programs to mitigate AMR in the GARP member network. These meetings see the participation of experts of diverse backgrounds, who through their professional experiences, suggest ways to make national immunization plans more robust and reduce AMR.
IN-PERSON WORKSHOPS
In-person, day-long workshops in GARP countries convene experts and policymakers from the AMR and immunization departments, the Ministry of Health, the Ministry of Finance, technical advisory groups of the government, academics, and representatives from international organizations working in the AMR and immunization space in these GARP member nations to present national-level evidence on the value of vaccines as a mitigation tool for AMR.
Publications
- GARP Pakistan Working Group. Situation Analysis Report on Antimicrobial Resistance in Pakistan: Findings and Recommendations for Antibiotic Use and Resistance; 2018. Available here.
- GARP Bangladesh Working Group. Antibiotic Use and Resistance in Bangladesh: Situation Analysis and Recommendations. Directorate General of Drug Administration; 2018. Available here.
- GARP Mozambique Working Group (B Sigaúque, E Sevene, co-chairs). Situation Analysis and Recommendations: Antibiotic Use and Resistance in Mozambique. Maputo: Manhiça Health Research Centre; 2015 July. 42 p. Available here.
- GARP Nepal National Working Group (B Basnyat, P Pokharel, co-chairs) Situation Analysis and Recommendations: Antibiotic Use and Resistance in Nepal. Kathmandu: Nepal Public Health Foundation; 2015 May. 20 p. Available here.
- GARP Tanzania National Working Group (S Aboud, R Mdegela, co-chairs) Situation Analysis and Recommendations: Antibiotic Use and Resistance in Tanzania. Dar es Salaam: Muhimbili University of the Health and Allied Sciences; 2015 June. 118 p. Available here.
- Uganda National Academy of Sciences (D Byarugaba, D Kusemererwa, co-chairs). Antibiotic resistance in Uganda: Situation analysis and recommendations. Kampala: Uganda National Academy of Science; 2015 Aug. 94 p. Available here.
- GARP Vietnam National Working Group (NV Kinh, chair). Situation Analysis: Antibiotic Use and Resistance in Vietnam. Hanoi: Oxford University Clinical Research Unit; 2010 Oct. 36 p. Available here.
- AG Duse (chairman) et al. Global Antibiotic Resistance Partnership—Situation analysis: antibiotic use and resistance in South Africa. Supplement to South African Medical Journal-Part 2: August 2011. 2011; 101(8):549–96. Available here.
- Global Antibiotic Resistance Partnership India National Working Group (NK Ganguly, Chairman) Situation Analysis: Antibiotic Use and Resistance in India. New Delhi: Center for Disease Dynamics, Economics & Policy; 2011 Mar. 74 p. Available here.
- GARP Kenya Working Group (S Kariuki, ed) Situation Analysis and Recommendations: Antibiotic Use and Resistance in Kenya. Nairobi: Kenya Medical Research Institute; 2012. 102 p. Available here.

This edition covers GARP workshops from 2023 through April 2024, the latest research on AMR and vaccines, and more.